7 results
Caring for Bierzo: A plan for improving motivation for health workers from Mental Health
- J. M. Pelayo-Terán, Y. Zapico-Merayo, S. Vega-García, M. E. García-Llamas, Z. Gutiérrez-Hervás, A. Castro-Bayón
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S309-S310
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Motivation is an essential determinant of performance, particularly for those working in difficult conditions, such as the conditions facing many health workers. The relationship between motivation and performance is influenced by the health workers’ organizational environment and social context. Many intrinsic and extrinsic factors may influence the impulse to head for and maintain and effort to achieve the objectives of the organization these may include acknowledgements, status and incentives, but also auto efficacy perception, personal growth, welfare and physical and mental health.
In the last years and particularly during COVID-19 pandemic health organizations have suffered a crisis of lack of motivation and high turnover rates in health professional, particularly among highly specialized professions.
Objectivesto develop a quality program to promote mental health and motivation, detect risk of mental disorders and improve communication skills in the health workers of the Health Area of El Bierzo (GASBI).
MethodsA committee with four members form the psychiatry and mental health service, two from the Quality and Security Unit and 1 from the Occupational Risk Prevention Service analyzed the GASBI with a SWOT-CAME matrix analysis. Actions to be implemented were ordered with a Hanlon method score according to a representative sample of the employees of GASBI.
ResultsThe CAME matrix recommended an offensive strategy, given a number of strengths and the opportunities for an administration sensible to new paradigms. The program proposed included 6 main lines (evaluation, access to mental health consultation, prevention of suicide behavior, resilience group, communication and relation groups and a group of actions to improve motivation and prevent burnout called “10 actions to dream together”, displayed in figures 1 and 2. The Hanlon classified suicide behaviour as the highest priority (score: 16,25 points), mental disorders the second (score: 13.75), then fatigue (13 p), burnout and resilience (12p) and the less prioritary was motivation (7 points). The project was displayed in a canvas business model (figure 3)
Image:
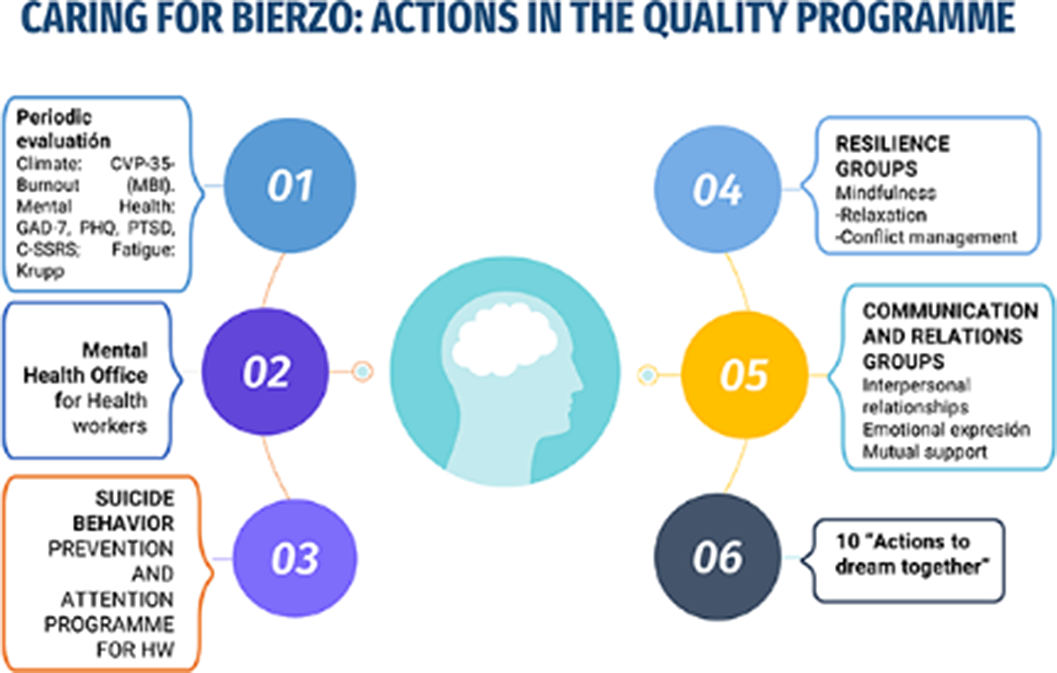
Image 2:

Image 3:
 Conclusions
ConclusionsMental health, fatigue, burnout and motivation of health workers is a complex problem that affect health organizations and quality of services. Mental Health service have an important role in the promotion of wellbeing and prevent burnout in the health system.
Disclosure of InterestNone Declared
Establishing priorities for a Mental Health strategy in Castilla y Leon: The cohesion of professionals and society
- J. M. Pelayo-Terán, Y. Zapico-Merayo, A. M. Saez Aguado, R. Villa Carcedo, Á. Álvaro Prieto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S540-S541
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The reform of mental health care is a key health policy target. Mental health care provision in Spain is designed with national and regional strategies that stablish the objectives to develop. The Castilla y Leon regional strategy 2022-2026 aim to stabilsh the priorities for objectives and actions with stakeholders from th eregional society.
ObjectivesTo evaluate priorities in the implementation of a Mental Health strategy with the consensus of professionals and society.
MethodsAn initial consensus was achieved with the regional health goverment and local mental health representatives, considering the 2022-2026 national strategy and other mental health plans from nearby regions. Lines in the strategy included transversal lines (part of all the mental health scope) and action lines (priorities focused in one relevant field)
Priorities were stablished by different representatives from mental health and other healthcare professionals, social and educational stakeholders, scientific societies, people with mental health disorders and families. After agreeing to participate in the process, they had to answer an online survey. For each line, they have to score from 0 to 10.
Results500 subjects participated (44% Healthcare workers, 5.8% education or social services, 3.8% Justice, 8,6% workers for associations, 14% Mental Health Care users). All the lines were highly appreciated (mean score >7). Within the transversal lines, the highest score was for the Humanization line (8.81±1.43) and the lowest for the Digitalization line (7.18±1.92). In the Action Lines, the highest score was for Suicide (9.03±11.5) and the lowest for Elder people (8.04±1.94).
Prevention line had higher scores by Education, Justice, Associations and Healthcare professionals and the lowest was for users (F: 2.754; p=0.012). In the Digitalization line the higher scores were in the health professionals and scientific societies and the lowest in the users (F:4.665; p<0.001). In the research, innovation and Training line, the higher scores were for professionals, societies and users and the lowest in the education and justice groups. The only differences found in the Action lines was for the Addiction line, with higher scores for societies, social services, professionals and users and lower in Associations and Justice (F:2.219; p=0,040)
Image:
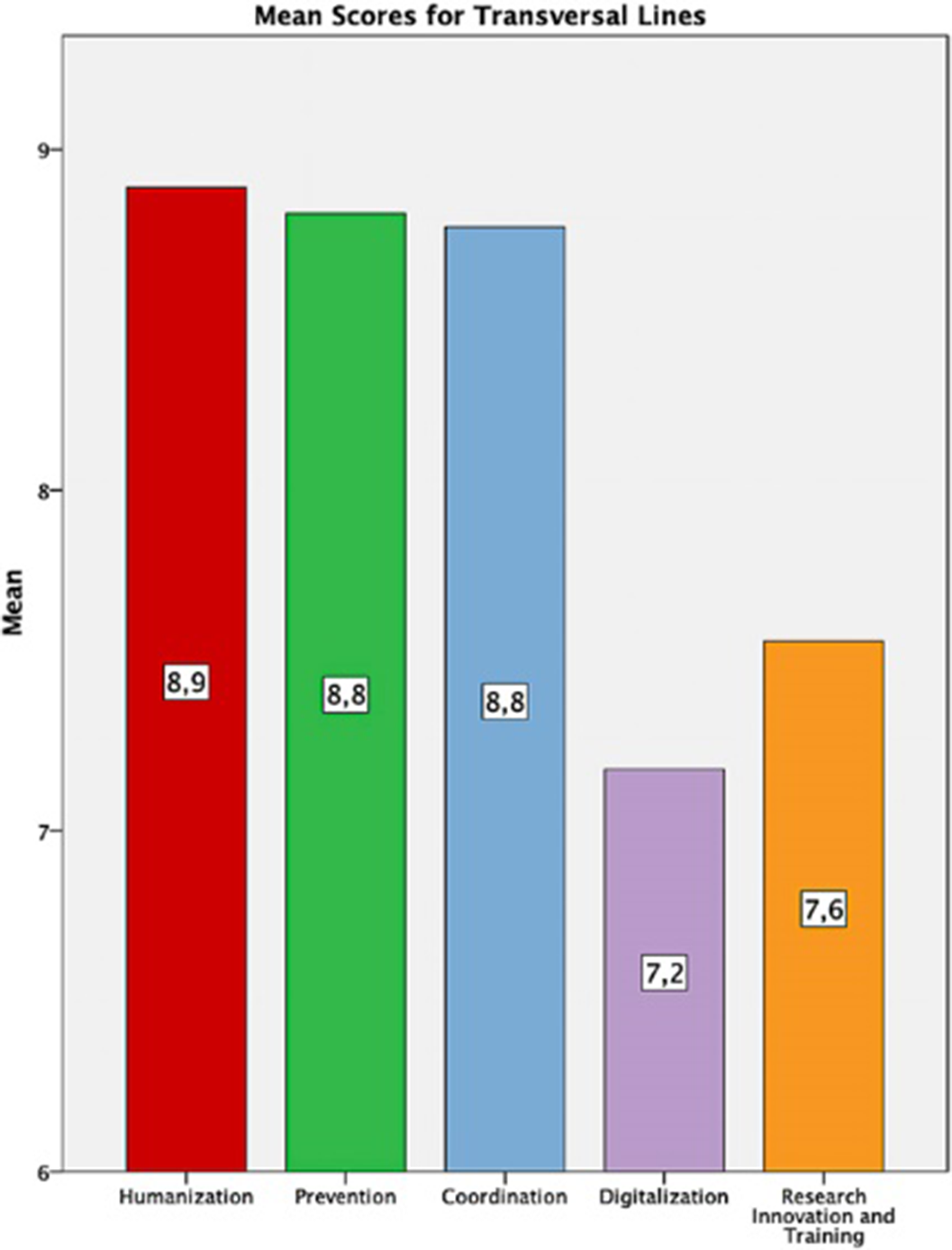
Image 2:
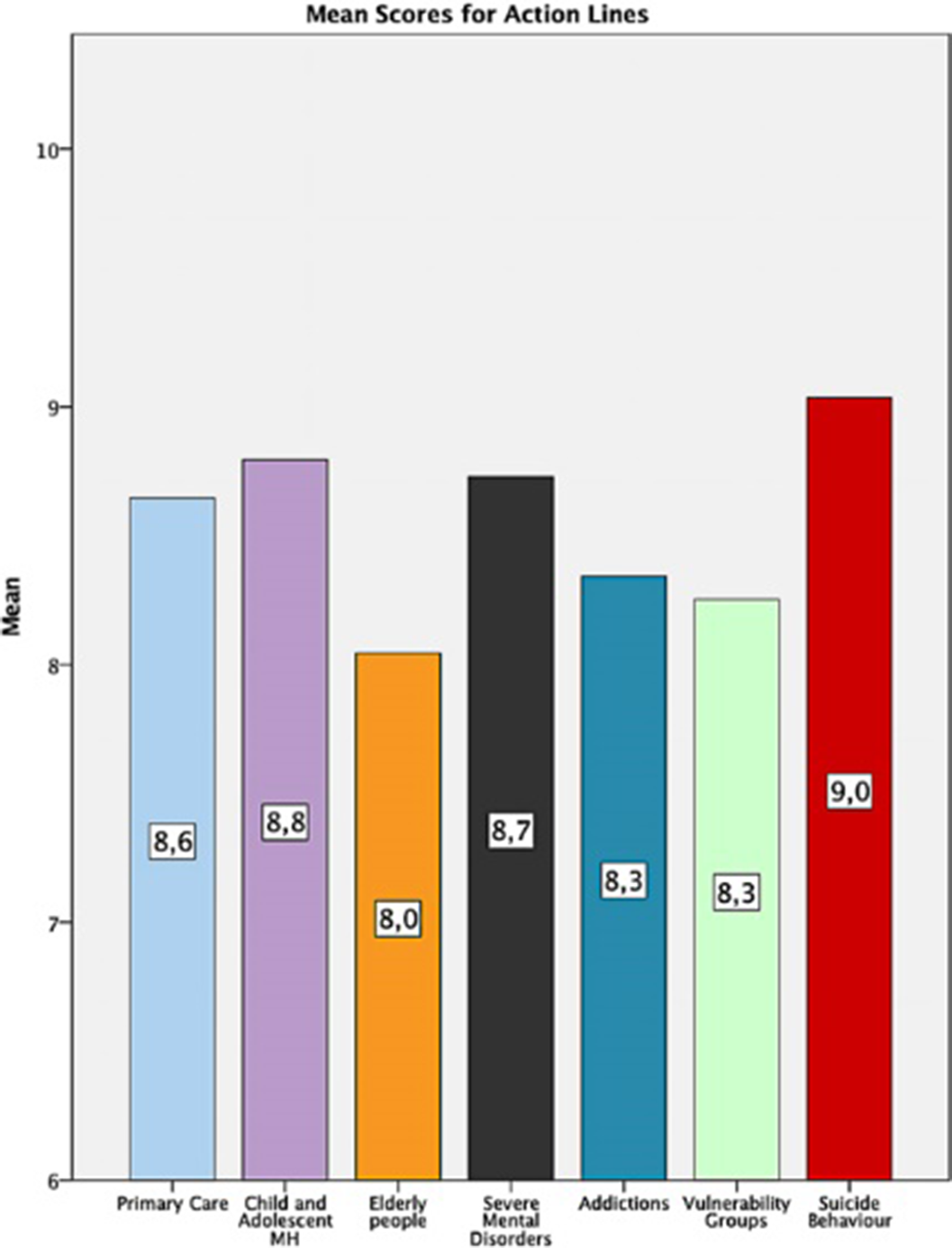 Conclusions
ConclusionsHighest transversal priority for the MH Strategy was Humanization of Mental Health Services, and the most critical action was Suicide prevention. Professionals, Scientific societies and Users considered more important research, innovation and training compared with other society groups, whereas the less important areas for the users were digitalization and prevention users. These priorities will help to design the implementation and schedule for the lines of the Mental Health Strategy in Castilla y León.
Disclosure of InterestNone Declared
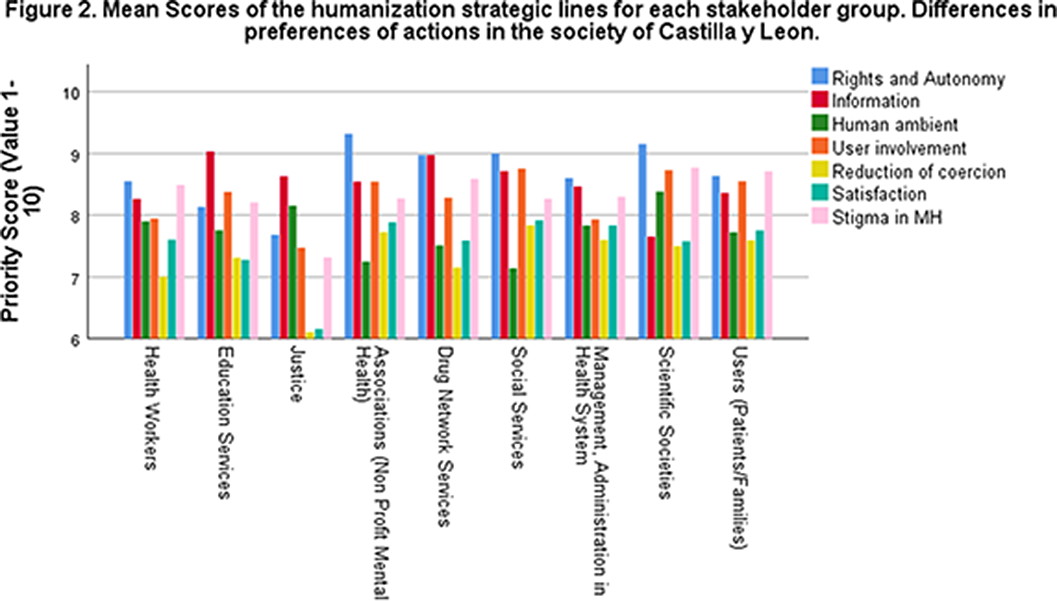
A social consensus to prioritize humanization strategies for Mental Health in Castilla y León
- J. M. Pelayo-Terán, Y. Zapico-Merayo, S. Vega-García, M. E. García-Llamas, Z. Gutiérrez-Hervás, A. Sáez-Aguado, M. R. Villa-Carcedo, A. Álvaro-Prieto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S908-S909
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Humanization in Mental Health is a concept that treat to conceal in the last decades the quality, efficiency and safety of care of complex diseases and conditions with individual values, needs and preferences and involves the patient and society in the decision-making priority.
Objectivesto stablish and evaluate the priorities of different groups of interest in the development of a new humanization plan for mental health
MethodsDuring 2022 a Humanization plan for the Spanish region of Castilla y Leon (2.400.000 habs) was developed with a Delphi model. Participants included 36 stakeholders including mental health services, administration, social services, associations, patients and families. They stablished 32 objectives distributed in 7 strategic lines: 1. “People First” (Rights, Autonomy and Information); 2. “From People to Services” (Participation of users in mental heal services); 3. “Person-Centered-Assistance” 4. “Processes sensible to change” (reduction of coercion); 5. “Human ambient” (Improvement of units, psychosocial interventions). 6. Innovation, training and climate (not evaluated here). 7. “People without marks” (battle against stigma).
Priorities in the lines were stablished by representatives from mental health and other healthcare professionals, social and educational stakeholders, scientific societies, patients and families. After agreeing to participate in the process, they had to answer an online survey. For each line, they have to score it from 0 to 10.
Results500 subjects participated (38.6% Healthcare workers, 14% Mental Health Care users, 9.8% Social Services, 8.8% Associations, 7.8% Drug Services 6% Management of Health System, 5.8% Education Services, 3.8 Justice). Humanization was the most appreciated plan within the mental health plan 2022-2026 in Castilla y Leon (8.81±1.43).
The Highest priority score was given to the Rights (8.68 + 1.54), Information (8.44 + 1.60) and Stigma (8.43 + 1.89) lines and the lowest were the evaluation of satisfaction (7.62 + 1.90) and Reduction of Coercion (7.29 + 2.12). Differences were found between groups. Scores in Rights and Autonomy (F:3.474; p<0.001) were highest in the Associations (9.32 +1.01) and lowest in the Justice group (7.68 + 1.67). In the information line the highest score (F:2.431; p=0,014) was in the Education Services (9.03 +0,94) compared to Scientific Societies (7,65 + 2,13). Highest score for Participation of Users (F:2,968; p=0,003) was in Social Services (8.76 +1.48) compared to Justice (7.47 +1.95). There were differences in the coercion reduction line (F:2.165; p=0,029) but no pairwise differences were found
Image:
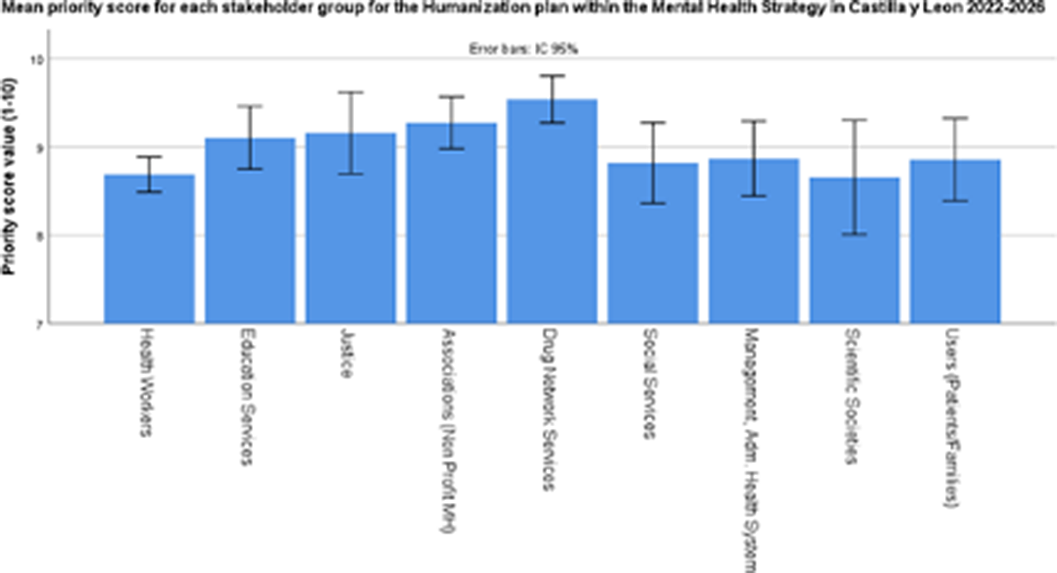
Image 2:
 Conclusions
ConclusionsHumanization approaches are well appreciated by different stakeholders. Priorities in our region start with rights, information and integration and mental health users in the health system and society
Disclosure of InterestNone Declared
Mental impact of Covid-19 among Spanish healthcare workers. A large longitudinal survey
- J. Alonso, G. Vilagut, I. Alayo, M. Ferrer, F. Amigo, A. Aragón-Peña, E. Aragonès, M. Campos, I. del Cura-González, I. Urreta, M. Espuga, A. González Pinto, J. M. Haro, N. López Fresneña, A. Martínez de Salázar, J. D. Molina, R. M. Ortí Lucas, M. Parellada, J. M. Pelayo-Terán, A. Pérez Zapata, J. I. Pijoan, N. Plana, M. T. Puig, C. Rius, C. Rodriguez-Blazquez, F. Sanz, C. Serra, R. C. Kessler, R. Bruffaerts, E. Vieta, V. Pérez-Solá, P. Mortier, MINDCOVID Working group
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 31 / 2022
- Published online by Cambridge University Press:
- 29 April 2022, e28
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Longitudinal data on the mental health impact of the coronavirus disease 2019 (Covid-19) pandemic in healthcare workers is limited. We estimated prevalence, incidence and persistence of probable mental disorders in a cohort of Spanish healthcare workers (Covid-19 waves 1 and 2) -and identified associated risk factors.
Methods8996 healthcare workers evaluated on 5 May–7 September 2020 (baseline) were invited to a second web-based survey (October–December 2020). Major depressive disorder (PHQ-8 ≥ 10), generalised anxiety disorder (GAD-7 ≥ 10), panic attacks, post-traumatic stress disorder (PCL-5 ≥ 7), and alcohol use disorder (CAGE-AID ≥ 2) were assessed. Distal (pre-pandemic) and proximal (pandemic) risk factors were included. We estimated the incidence of probable mental disorders (among those without disorders at baseline) and persistence (among those with disorders at baseline). Logistic regression of individual-level [odds ratios (OR)] and population-level (population attributable risk proportions) associations were estimated, adjusting by all distal risk factors, health care centre and time of baseline interview.
Results4809 healthcare workers participated at four months follow-up (cooperation rate = 65.7%; mean = 120 days s.d. = 22 days from baseline assessment). Follow-up prevalence of any disorder was 41.5%, (v. 45.4% at baseline, p < 0.001); incidence, 19.7% (s.e. = 1.6) and persistence, 67.7% (s.e. = 2.3). Proximal factors showing significant bivariate-adjusted associations with incidence included: work-related factors [prioritising Covid-19 patients (OR = 1.62)], stress factors [personal health-related stress (OR = 1.61)], interpersonal stress (OR = 1.53) and financial factors [significant income loss (OR = 1.37)]. Risk factors associated with persistence were largely similar.
ConclusionsOur study indicates that the prevalence of probable mental disorders among Spanish healthcare workers during the second wave of the Covid-19 pandemic was similarly high to that after the first wave. This was in good part due to the persistence of mental disorders detected at the baseline, but with a relevant incidence of about 1 in 5 of HCWs without mental disorders during the first wave of the Covid-19 pandemic. Health-related factors, work-related factors and interpersonal stress are important risks of persistence of mental disorders and of incidence of mental disorders. Adequately addressing these factors might have prevented a considerable amount of mental health impact of the pandemic among this vulnerable population. Addressing health-related stress, work-related factors and interpersonal stress might reduce the prevalence of these disorders substantially. Study registration number: NCT04556565
Trajectories of symptom dimensions in short-term response to antipsychotic treatment in patients with a first episode of non-affective psychosis
- J. M. Pelayo-Terán, F. J. Diaz, R. Pérez-Iglesias, P. Suárez-Pinilla, R. Tabarés-Seisdedos, J. de León, B. Crespo-Facorro
-
- Journal:
- Psychological Medicine / Volume 44 / Issue 1 / January 2014
- Published online by Cambridge University Press:
- 06 March 2013, pp. 37-50
-
- Article
- Export citation
-
Background
Trajectory patterns of positive, disorganized and negative dimension symptoms during antipsychotic treatment in drug-naive patients with first-episode psychosis have yet to be examined by using naturalistic data.
MethodThis pragmatic clinical trial randomized 161 drug-naive patients with a first episode of psychosis to olanzapine, risperidone or haloperidol. Patients were assessed with the Scale for the Assessment of Negative Symptoms (SANS) and Positive Symptoms (SAPS) at baseline and at the end of weeks 1, 2, 3, 4 and 6 of antipsychotic treatment. Censored normal models of response trajectories were developed with three dimensions of the SAPS-SANS scores (positive, disorganized and negative) in order to identify the different response trajectories. Diagnosis, cannabis use, duration of untreated psychosis (DUP), smoking and antipsychotic class were examined as possible predictive variables.
ResultsPatients were classified in five groups according to the positive dimension, three groups according to the disorganized dimension and five groups according to the negative dimension. Longer DUPs and cannabis use were associated with higher scores and poorer responses in the positive dimension. Cannabis use was associated with higher scores and poorer responses in the disorganized dimension. Only schizophrenia diagnosis was associated with higher scores and poorer responses in the negative dimension.
ConclusionsOur results illustrate the heterogeneity of short-term response to antipsychotics in patients with a first episode of psychosis and highlight markedly different patterns of response in the positive, disorganized and negative dimensions. DUP, cannabis use and diagnosis appeared to have a prognostic value in predicting treatment response with different implications for each dimension.
Cannabis abuse is associated with decision-making impairment among first-episode patients with schizophrenia-spectrum psychosis
- I. Mata, J. M. Rodríguez-Sánchez, J. M. Pelayo-Terán, R. Pérez-Iglesias, C. González-Blanch, M. Ramírez-Bonilla, O. Martínez-García, J. L. Vázquez-Barquero, B. Crespo-Facorro
-
- Journal:
- Psychological Medicine / Volume 38 / Issue 9 / September 2008
- Published online by Cambridge University Press:
- 16 November 2007, pp. 1257-1266
-
- Article
- Export citation
-
Background
Cannabis use appears to be a risk factor for schizophrenia. Moreover, cannabis abusers show impaired decision-making capacities, linked to the orbitofrontal cortex (OFC). Although there is substantial evidence that first-episode schizophrenia patients show impairments in cognitive tasks associated with the dorsolateral prefrontal cortex (DLPFC), it is not clear whether decision making is impaired at schizophrenia onset. In this study, we examined the association between antecedents of cannabis abuse and cognitive impairment in cognitive tasks associated with the DLPFC and the OFC in a sample of first-episode patients with schizophrenia-spectrum disorders.
MethodOne hundred and thirty-two patients experiencing their first episode of a schizophrenia-spectrum psychosis were assessed with a cognitive battery including DLPFC-related tasks [backward digits, verbal fluency (FAS) and the Trail Making Test (TMT)] and an OFC-related task [the Iowa Gambling Task (GT)]. Performance on these tasks was compared between patients who had and had not abused cannabis before their psychosis onset.
ResultsNo differences were observed between the two groups on the performance of any of the DLPFC-related tasks. However, patients who had abused cannabis before their psychosis onset showed a poorer total performance on the gambling task and a lower improvement on the performance of the task compared to no-abusers.
ConclusionsPre-psychotic cannabis abuse is associated with decision-making impairment, but not working memory and executive function impairment, among first-episode patients with a schizophrenia-spectrum psychosis. Further studies are needed to examine the direction of causality of this impairment; that is, does the impairment make the patients abuse cannabis, or does cannabis abuse cause the impairment?
Pretreatment predictors of cognitive deficits in early psychosis
- C. González-Blanch, B. Crespo-Facorro, M. Álvarez-Jiménez, J. M. Rodríguez-Sánchez, J. M. Pelayo-Terán, R. Pérez-Iglesias, J. L. Vázquez-Barquero
-
- Journal:
- Psychological Medicine / Volume 38 / Issue 5 / May 2008
- Published online by Cambridge University Press:
- 09 October 2007, pp. 737-746
-
- Article
- Export citation
-
Background
Predicting cognitive deficits in early psychosis may well be crucial to identify those individuals most in need of receiving intensive intervention. As yet, however, the identification of potential pretreatment predictors for cognitive performance has been hampered by inconsistent findings across studies. We aimed to examine the associations of functional and clinical pretreatment variables with cognitive functioning after a first psychotic episode.
MethodOne hundred and thirty-one patients experiencing first-episode psychosis were assessed for psychopathology, pre-morbid functioning, duration of illness, age of onset, and family history of psychosis and neurocognitive functioning. Multiple regression analyses were conducted for six basic cognitive dimensions known to be affected in this population: verbal learning, verbal memory, verbal comprehensive abilities, executive functioning, motor dexterity and sustained attention.
ResultsPre-morbid functioning was the main predictor for five out of the six basic cognitive domains. Pre-morbid social adjustment difficulties were associated with worse performance in executive functioning, motor dexterity and sustained attention. Academic functioning was associated with verbal comprehension, and verbal learning and memory. Gender, age of onset, duration of untreated psychosis, and family history of psychosis had no or limited value as predictors of neurocognitive outcome.
ConclusionsPoor pre-morbid functioning was related to a worse performance in the six basic cognitive dimensions evaluated; however, this accounted for only a small amount of the explained variance. Cognitive impairment is a prominent feature in patients with early psychosis regardless of favorable prognostic features such as short duration of illness, female gender, later age of onset, and non-family history of psychosis.










